-
Programs
Associate DegreeBachelor DegreePathways
-
Admissions & Aid
AdmissionsFinancial Aid
-
Offices & Services
Human ResourcesInfo & Help Desk
- Blog
- Giving
- Home
- Programs & Degrees
Programs
NURSING OPTIONS

Associate of Science in Nursing (ASN)
A fast, flexible route to your RN credential.
- 2 years to complete
- In-person
- Associate degree
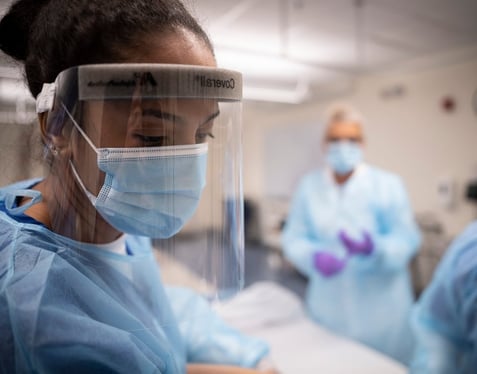
LPN to RN: Advanced Placement
- 2 years to complete
- In-person
- Associate degree
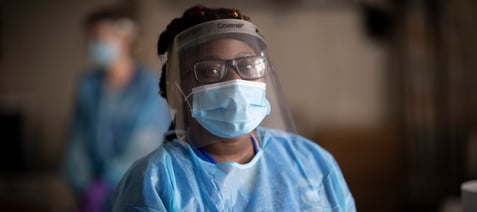
Nursing: RN-to-BSN
Ranked #1 in best RN-BSN program in MA by RegisteredNursing.org
- 16 months to complete
- 100% Online
- Bachelor degree
HEALTHCARE OPTIONS
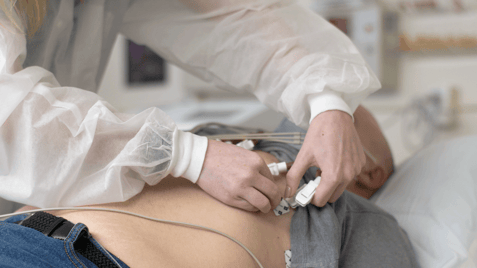
EKG Certificate
Electrocardiography training in 15 weeks.
- 4 months to complete
- Hybrid
- Certificate
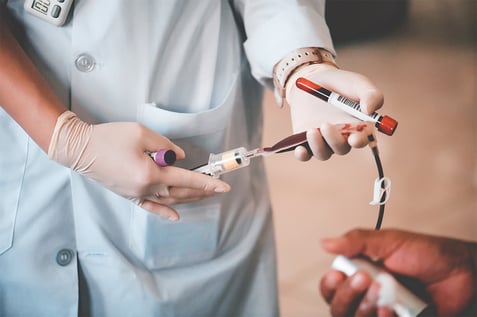
Phlebotomy Certificate
Phlebotomy training for college credit.
- 4 months to complete
- Hybrid
- Certificate

Health Science
Start building your strong foundational knowledge of healthcare delivery.
- 2 years or less to complete
- 100% Online /or/ Hybrid
- Associate degree

Healthcare Administration
Take the next step toward a leadership or management position in healthcare in less than two years.
- 2 years or less to complete
- 100% Online
- Bachelor degree
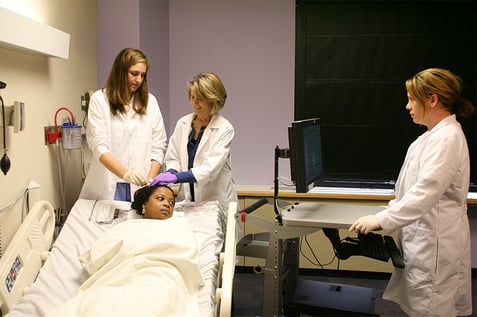
Neurodiagnostic Technology
Change your career online in one year.
- 12* months to complete
- Hybrid
- Certificate

- 2 semesters to complete
- Hybrid
- Certificate
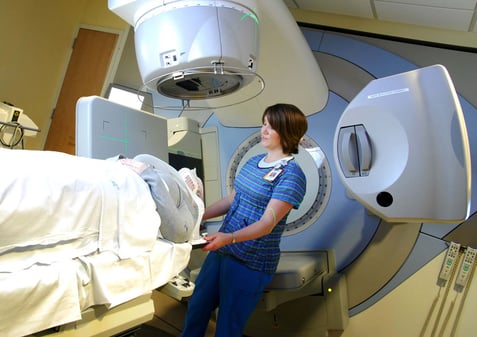
Radiation Therapy
Radiation therapists help one patient at a time fight cancer by administering radiation treatments.
- 2 to 3 years to complete
- In-person
- Associate degree
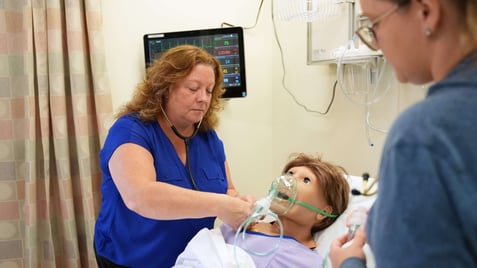
Respiratory Care
Respiratory therapists help patients who have difficulty breathing.
- about 2 years to complete
- Hybrid
- Associate degree
ALUMNI STORIES

“As soon as I got to Labouré, I loved the school and I loved the teachers. You’re able to ask questions. I find myself growing at Labouré.”
© 2023 Labouré College of Healthcare. All Rights Reserved.