-
Programs
Associate DegreeBachelor DegreePathways
-
Admissions & Aid
AdmissionsFinancial Aid
-
Offices & Services
Human ResourcesInfo & Help Desk
- Blog
- Giving

Educating the next generation of healthcare providers.
Like you, our students are adults juggling many responsibilities. Labouré provides the flexibility and support you need to succeed. Invest in your education and care for your future.
OUR PROGRAMS
A career that makes a difference
Our mission is to educate the diverse, compassionate, and highly skilled healthcare professionals that our communities need.
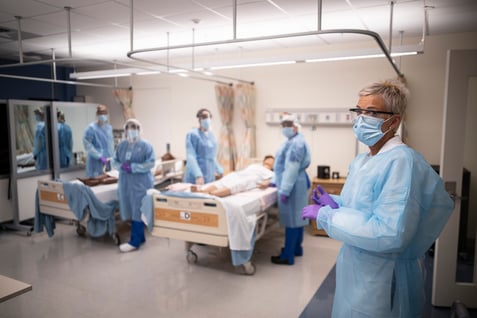
Nursing Pathways
Nursing is a rewarding career in caring for others, with many pathways and credentials a nurse can earn along the way. Some start out as certified nursing assistants (CNAs), or licensed practical nurses (LPNs), while others start as registered nurses (RNs) or registered nurses with a BSN.
We can help you find the right path for you, whether you're just starting out or looking to take your credentials to the next level.

Healthcare Pathways
The healthcare industry represents a wide variety of skills from front-line patient care to business operations, and everything in between. With so many entry points and certifications available, the path you take can be up to you, and your career opportunities are limitless.
Whether you’re just starting out in the healthcare field, or taking the next step in your career, we can help you find the program that’s right for you. You can explore our program options below.
Stats
Personally and financially rewarding careers
SPOTLIGHT
Choosing the Right Healthcare Career for You

Video Reel
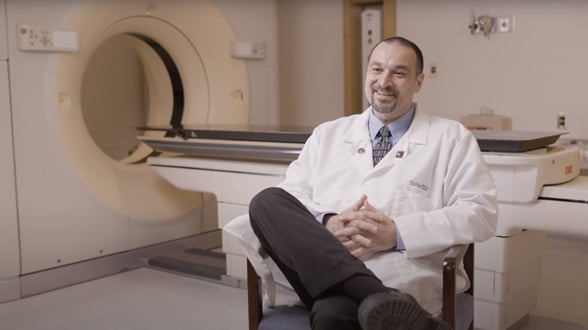
Sean O'Leary, RTT '93
Sean is a 2017 recipient of Labouré College’s Mass Care Award, now the Nurse Impact Awards. He is the Chief Radiation Therapist at Tufts Medical Center.
Giving
Support the men and women who will one day care for us.

When you support Labouré students, you’re supporting the professional advancement, economic independence, and personal empowerment of the people who are ready to go to work building a healthier future.
One nurse will care for thousands. Your gift makes that possible.
Care for your future.
© 2023 Labouré College of Healthcare. All Rights Reserved.
